
The Society for Family Health serves as a prime recipient for the Key Populations Programtitled, HIV prevention for Key Populations since 2011 with funding from USAID. With 7 sub-recipients predominantly KP-led organizations, the program is implemented in 6 sites – Keetmanshoop, Katima Mulilo, Windhoek, Oshakati, Walvis Bay/Swakopmund and Oshikango.
In Namibia, the data from the Integrated Bio Behavioral Surveillance Study (IBB SS) conducted in 2012/13 suggests HIV prevalence among Female Sex Workers (FSWs) was higher than females in the general population while prevalence among Men who have Sex with Men (MSM) was comparable to men from general population in regions studied except Windhoek were the prevalence was almost double that of men in general population.
The term Key Populations vs Most at risk populations
The term ‘key population’ has gained more popularity compared to the earlier term – Most at Risk Population (MARPS) that put together sub- groups that were determined to be at a higher risk of HIV infection by the nature of their behavior, lifestyle or circumstances. This new term is viewed as a more accurate and less stigmatizing description because it seeks to describe the risk factor as opposed to population groups.
In this way MSM or ‘men who have sex with men’ is more accurate than ‘Gay men’ because one could self-describe as Gay but not necessarily be engaging in high risk behavior. In the context of this KP program, populations that are referred to as key populations herein include, Men who have sex with Men (MSM), Female Sex Workers (FSW) and Transgender (TG) women.
Specific objectives of the program:
- Improved access to a core set of HIV prevention, care and treatment interventions to reduce HIV transmission among Key Populations;
The core of KP program is case management which aims to provide holistic and comprehensive care to KPs including effective linkages to services. The Care Cascade ensures comprehensive management of clients seeking services and it enforces the 90-90-90 Global Strategy to reduce HIV Infections and death. This approach is implemented at all sites: Keetmanshoop, Windhoek, Walvis Bay/ Swakopmund, Oshakati, Oshikango and Katima Mulilo.
- The following local 7 organizations which are predominately KP-led are the implementing partners:
- Out-Right Namibia (ORN),
- Rights Not Rescue Trust (RNRT),
- Kings Daughters Organization (KDO),
- Voice of Hope Trust (VHT),
- Caprivi Hope for Life (CHFL),
- Namibia Planned Parenthood Association (NAPP A) and
- Walvis Bay Corridor Group’s Wellness Program (WBCG).


Through this process of case management, clients are provided with information about HIV awareness, risk reduction HIV Testing, enrollment on ART and other services, and facilitating a process to ensure they remain negative. Pre-Exposure Prophylaxis (PrEP) provision and HIV Self-Testing are added components to the program as part of the combination prevention approach.
The Key Populations program is helping to achieve the HIV epidemic control through the following initiatives
- Expand access, utilization and quality of HIV prevention, care and treatment interventions to achieve HIV epidemic control
- Provide a combination prevention package including sexual risk reduction counseling and condom/lubricant distribution
- Conduct targeted HIV testing and counseling (HTC) services using standard and novel approaches in community and facility settings
- Provide oral pre-exposure (PrEP) and post exposure (PEP) ARV prophylaxis as additional prevention tools
- Ensure Effective sexually transmitted infection screening, diagnosis and treatment services
- Provide Integrated TB/HIV care and treatment including antiretroviral therapy (ART) for intended populations consistent with national guidelines for adults and adolescents
- Assist key population-led local civil society organizations to contribute to HIV epidemic control
- Improve the enabling environment for HIV-related policies, operational guidelines, data collection and analysis and service delivery by all stakeholders of key populations
Highlight of Achievements:
- For 2017 over 7,000 key populations have accessed HIV testing services and know their status of which 39% are new testers
- Peer-driven outreach activities yield better results in facilitating access and building trust in the program
- Striving towards narrowing the gap between HIV diagnosis and linkage to ART
- Linkage to ART among key populations is almost is above 70% against target and aim to close this gap in the coming year
The chart below indicates that KPs that tested between Oct – Dec 2017, only 159 (9%) out of 1,732 KPs tested. Of those that tested positive, 41% tested less than 12 months followed by 36% that tested 12 months ago, while 24% tested for the first time. This data illustrates that more efforts need to be made to find more KPs that have never tested with the purpose of ensuring that they are immediately linked to treatment and other prevention services.
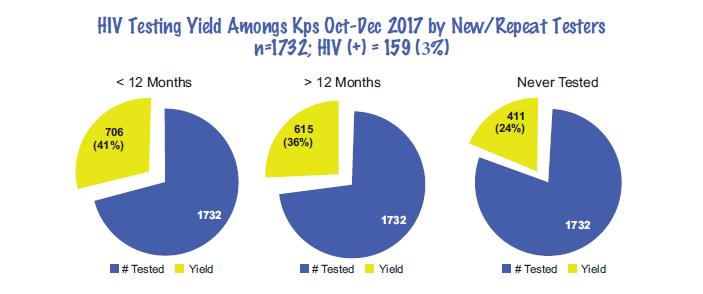
HIV Self Testing
The graph below shows that over 7,000 KP received HIV Testing Services (HTS) during this period. However, the program will continue to find the best approaches to ensuring that those testing positive are immediately linked to treatment.
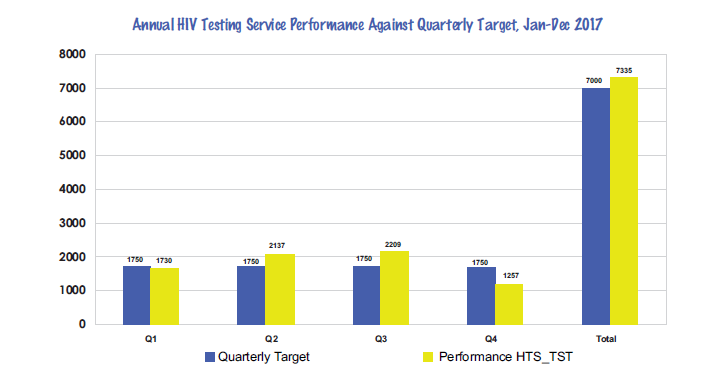
Access to HIV treatment
The chart below shows the number of KPs that were enrolled on ART against the target. Performance was below with 27%. Linkage to treatment following diagnosis pose challenges sometimes especially when HIV diagnosis was made through outreach services as clients need to visit the health facility for treatment. Delays in reaching the health facility and loss to follow up (inability to access the clients through mobile contacts provided or incorrect residential area), are some of the contributing factors in ensuring effective and prompt linkage to treatment. Also, ensuring that ART is provided on the mobile van would also increase linkage to treatment.
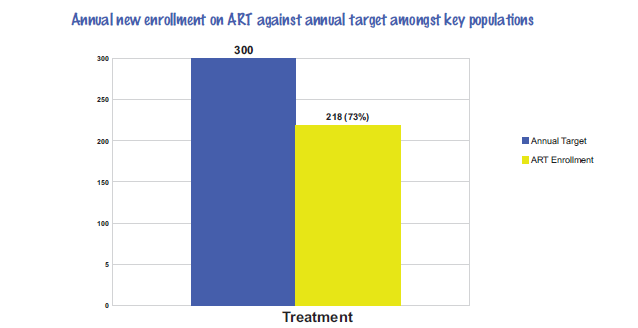
Challenges addressed;
- If non-sensitized health care providers engage these referrals, then negative experiences of clinical services by KPs could damage future recruitment and retention. Health care provider training for both sensitization and clinical competency is essential across not only at NAPPA and WBCG but also a select number of public clinics that are serving KPs.
- Meaningful opportunities to have key populations’ input in how services are delivered, improved and evaluated – through the national KP Technical working group and the regional stakeholders forums
- Support from trained peers who can help key populations access HIV testing and counseling and other HIV services


Lessons learnt:
- Empowered KPs can aid interactions with hidden and hard-to-reach members that have weak or no links to the HIV cascade.
- The introduction of CM implemented through case workers has resulted in steady improvements in HTC, documentation and LTC and enrollment of KPs on ART. Thus CM approach has proved effective in identifying, enrolling and linking KPs to essential services as part of the minimum package
- Scaling up CM through strategic deployment of case workers is needed to facilitate comprehensive HIV services and improve health outcomes for KPs. In order to sustain these efforts, it is crucial to ensure government buy in and support.
wordpress theme by initheme.com


2 comments. Leave new
I was wondering if you e’er considered dynamic the plaything of your parcel? Its really fortunate scripted; I pair what youve got to say. But maybe you could a little more in the way of proportion so grouping could unite with it ameliorate. Youve got an dreadful lot of schoolbook for only having one or 2 pictures. Maybe you could grapheme it out fitter? https://www.embromix.com
I was wondering if you ever advised dynamic the toy of your parcel? Its real easily return; I mercifulness what youve got to say. But maybe you could a infantile statesman in the way of accrual so grouping could connectedness with it modify. Youve got an terrible lot of schoolbook for alone having one or 2 pictures. Maybe you could type it out modify? https://www.embromix.com